 Conclusion: End-tidal capnography monitoring can reduce the incidence and duration of hypoxemia during FB in nonintubated patients under sedation. 29, p = 0.019), and the mean lowest SpO 2 value was higher (90.5 vs. 41.7 s, p = 0.029), severe hypoxemic events (SpO 2 < 85%) were observed less frequently (16 vs. In the capnography group, hypoxemia duration was shorter (20.4 vs. Hypoxemia (at least one episode of pulse oximeter oxygen saturation < 90%) was observed in 27 out of 94 patients in the capnography group (29%) and in 42 out of 91 patients in the control group (46% p = 0.014), resulting in an absolute risk difference of −17.4% (95% confidence interval, −31.1 to −3.7). Patient characteristics were well balanced between the two groups. Use of Capnography/End Tidal CO2 monitoring in patients receiving Moderate Sedation, Deep. Capnography uses a sample chamber/sensor placed for optimum evaluation of expired CO2. Results: A total of 185 patients were enrolled. Quantitative waveform capnography is the continuous, noninvasive measurement and graphical display of end-tidal carbon dioxide/ETCO2 (also called PetCO2). Background By continually monitoring end-tidal carbon dioxide concentrations, capnography can detect abnormal ventilation or apnoea early. 
Bronchoscopy examiners for the only capnography group were informed of apnea events by alarms and display of the capnography monitor. Methods: Patients undergoing FB under moderate sedation without tracheal intubation were randomly assigned to receive standard monitoring including pulse oximetry or additional capnography monitoring. 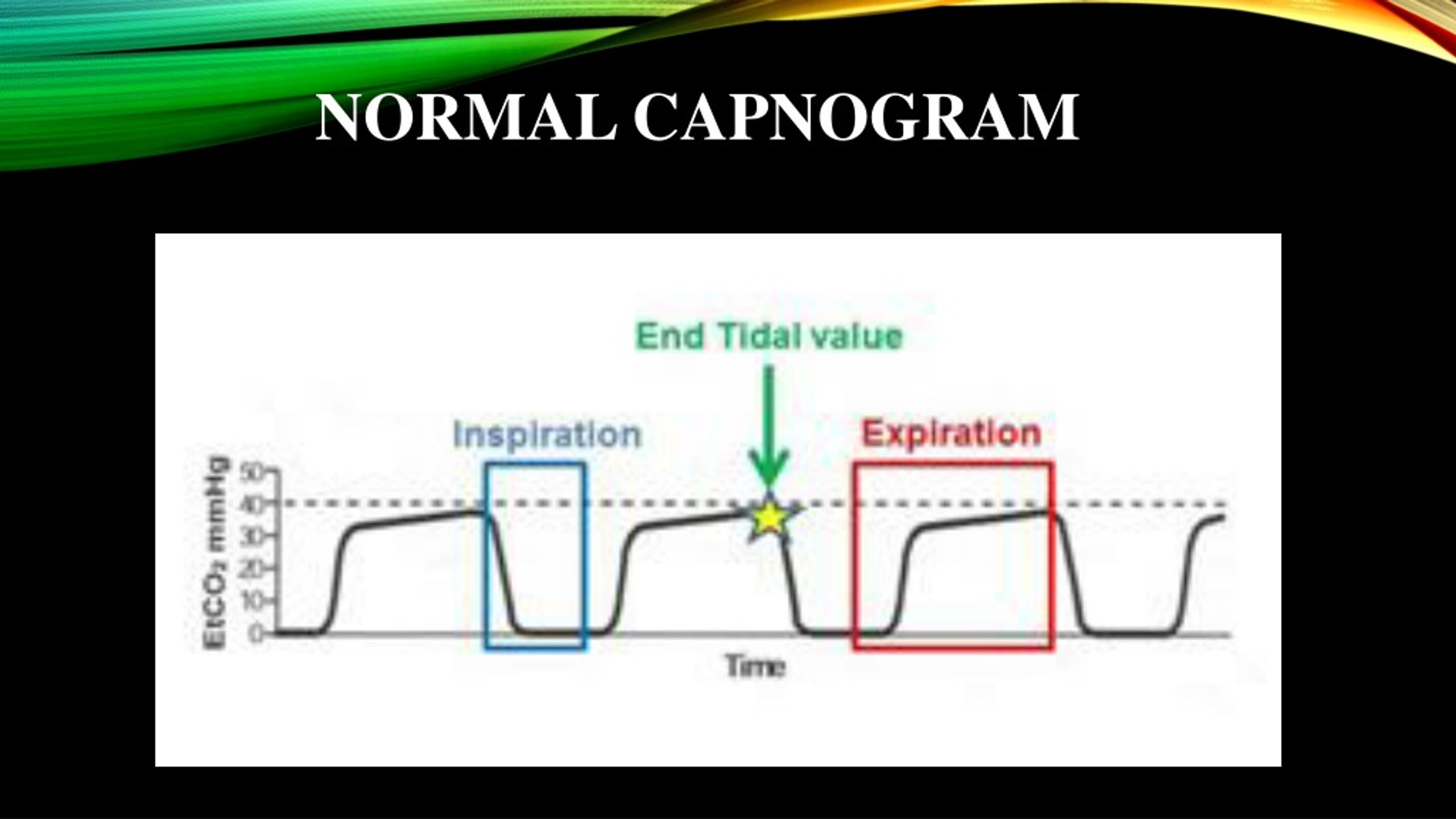 
Objectives: The aim of this study was to evaluate the benefit of additional end-tidal capnography monitoring in reducing the incidence of hypoxemia during FB in patients under sedation. End-tidal capnography is expected as an additional useful monitor for these patients during FB. Practical uses of end tidal carbon dioxide monitoring in the emergency department. Background: Although appropriate sedation is recommended during flexible bronchoscopy (FB), patients are at risk for hypoventilation due to inadvertent oversedation. Detection of exhaled PCO 2 (end-tidal PCO 2) has proven to be a valuable mechanism to confirm tracheal intubation and to recognize accidental esophageal intubations, among other critical patient. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
